|
Web Exclusives: PAWPLUS
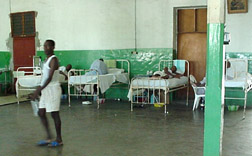
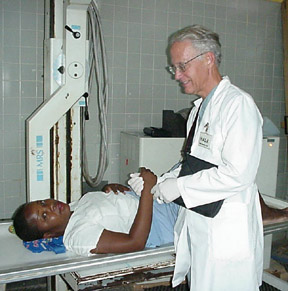
A Call to Care One medical missionary's account of a trip to Hopital Lumiere in Haiti
By Bill Greene '68
On Wednesday night I was alone on rounds when a nurse called, "Doctor, come quickly to the pediatric ward." A four-year-old child, who had been admitted for a hernia repair the next morning, was unconscious in respiratory distress. I went running, but was inwardly frightened. I have not studied pediatrics in 30 years. When I arrived the little girl was unconscious. We gave the her oxygen, but I felt helpless. Our first medical dictum kept running through my mind: Primum non nocere. I prayed that someone who knew what to do would soon arrive, but no one did. The lights kept going off, and we worked by flashlight. Two weeks before my trip, I had attended a refresher course on advanced cardiac life support. I clearly remembered that codes generally are called on adults for cardiovascular disease. Children, however, die more often from respiratory distress, so I knew that this was a critical situation. I recognized that the child suffered from bronchospasm. In retrospect, she had been given intravenous fluids that were probably outdated and contaminated. Her pulse oximeter dropped to 75. I had not choice but to do something. Without knowing the pediatric doses, I titrated small amounts of epinephrine intravenously. Slowly she responded. Later, the internist arrived; he had nothing further to recommend for the child. The next morning, when I made my rounds, she was smiling with her mother. I knew that she was one of the reasons I answered the call to be in Haiti. My journey to the island of Hispaniola began more than two years ago. After 23 years in a satisfying urology practice, I began to feel a sense of frustration and a lack of fulfillment in my daily routines. In retrospect, I know that was a very gentle call to search in another direction. After a year of investigation, I read an article in the Bulletin of the American College of Surgeons by Dr. Doug Soderdahl. At the age of 56, he retired from his urology practice to do full-time missionary work. His wife is his scrub nurse, and they travel the world together, treating the poorest of the poor and teaching urologic surgery skills to general surgeons. At the American Urological Association national meeting in Dallas, I shared a room with this marvelous missionary, who has become my mentor. Initially I was hesitant to commit to similar work. There seemed to be so many uncertainties, so many dangers. During that week of discussion and reflection, my confidence and enthusiasm grew. One memorable morning while in prayer, I came to the realize that, if God calls one to service, He will take care of the danger; there is no reason to be fearful of the unknown. I have since learned that He also will provide peace and gratification, far more generously than the secular world. My commitment was secure that day, but it took another year to find the right opportunity. I have talents in urology, which cannot be adequately utilized working out of a tent or the back of a truck. Dr. Joe Jarrett, an orthopedic surgeon in my community, had been to Haiti twice. He asked if I would like to join him on his next trip. After seeing his slide presentation, I knew this was the right opportunity. Preparing for the trip, set for August 26 through September 3, 2000, required a lot of hard work. Most important, I set out to beg for the people of Haiti, for the medical supplies and equipment that would be needed. I was overwhelmed by generosity: Not one person or company I solicited refused to participate, and most responded far more generously than I ever would have expected: Indigo Laser, Johnson & Johnson loaned a $54,000 laser and donated $12,000 in laser fibers to treat benign prostatic hypertrophy. Olympus loaned $20,000 worth of endoscopic equipment. Valley Lab loaned a $7,000 electrocautery unit. Eli Lilly donated over $800 in medications. Interchurch Medical Assistance and MAP International provided $10,000 in medication at a cost of $1,200. The Myrtle BeachRotary Clubs underwrote these expenses. My hospital, Grand Strand Regional Medical Center, offered to give us whatever we requested. The list of benefactors goes on and on. A heart-warming experience came from Oregon. Months before the trip I wanted to purchase some meaningful gifts for people who extended a special effort in helping me on my mission. I realized how useful my Leatherman Tool is to me. This is a wonderfully engineered instrument similar to a Swiss Army Knife; it is a complete tool box in a single instrument that I can't live without. It retails for $40. I wrote the president of the company, Timothy Leatherman. I explained my medical mission and asked if I could purchase a half dozen of his valuable tools as gifts, at a wholesale price. Three weeks later he wrote back that he could not provide tools at a wholesale price, but he enclosed two dozen of his tools for my journey. In order for a trip like this to take place, there are so many details that must fall into place. I am blessed with surgical training and skills, and the desire to share my talents with others. I needed and received the support of my wife and my daughter. They probably thought Dad was a bit crazy, but did not object. My practice needed coverage in my absence; fortunately I have five partners to take over the workload. I would need to shoulder the expenses for the trip. This was not a significant problem and, to my surprise, I received financial support from sources I did not even request. Although Hurricane Debbie threatened our travel plans, we set out at 4:15 a.m. on the most miserable journey I have ever made. I was accompanied by Dr. Jarrett, Dr. Cal Cunningham, an otorhinolaryngologist, and Donnie Long, an orthopedic operating room technician. Our first concern was our baggage; we had 14 large boxes and duffle bags, far more than the airlines allowed. When the attendant read we were medical missionaries, he loaded all the bags without comment. When we arrived in Atlanta, the agent learned of our mission and gave us first class accommodations, including a delicious breakfast (the last meal we could refer to as delicious). In preparation for the journey, I brushed up on French, which I had studied 30 years earlier in college. Although Creole is the language of the people of Haiti, French is the second tongue of the educated. On the flight from Miami, I had the opportunity to talk with a native Haitian school teacher who did not speak English. I learned from her that Haiti is an extremely poor country; due to decades of political corruption, no significant industry has survived, and infrastructure has deteriorated. Per capita income is $500 per year. Life expectancy is 51 years. Haiti has the highest HIV rate in the western hemisphere. Two-thirds of the people are illiterate and 60% go to bed hungry each night. Medical care is primitive, relying upon itinerant specialists to support the work of Haitian-trained primary care physicians and missionaries. The frightening part of the journey awaited us at the airport in Port au Prince. Groups of baggage attendants/gangsters fought to grab our bags. It was customary to expect one American dollar each time an attendant touched a travel bag. We could see our valuable cargo going off in many different directions. We had to fight back to avoid losing everything. We learned on our departure that the Haitian airport is the least secure airport in the entire world. It took six hours in a truck with a very aggressive driver, to travel 120 miles to the village of Bonne Fin and Hopital Lumiere. The roads in some areas were paved; in many areas they were washed-out river beds with deep ditches and football-size rocks. Our driver would weave from one side of the road to the other; he took us down paths that were never meant for motorized vehicles. We barely missed hitting pedestrians, bicycles, and animals along the path. We witnessed almost indescribable poverty. People lived in shanties with slabs of tin as roofs and plywood or branches for walls. Each village had a central well; water was carried on the top of the women's heads to the homes. Garbage covered the island, and the air had the stench of charcoal burning everywhere we went. We had taken our immunizations and malaria pills. We were warned not to drink the water, and we took Pepto-Bismol to avoid traveler's diarrhea. The hospital was in the village of Bonne Fin (translated this means "Happy Ending," which was what we experienced in our journey, 16 hours after we set out). It was developed by a general surgeon, Dr. Nelson from California in 1973. It would be considered outdated by U.S. standards, but was a monumental effort to build in a Third World country. The compound was protected by a tall brick wall and guards armed with rifles. Our residence was a cinder block building with non-potable, cold running water and electricity during daylight hours. The utilities in the compound were interrupted many times each day. We had plenty of roaches and lizards sharing the quarters. Food was basic but satisfying. My most memorable meal consisted of mashed potatoes, rice, French fries, and bread. We had chicken a few times, and I really developed a liking for goat meat. It tasted like barbecued pork, but was tougher and less greasy. Our most valuable possessions were vinyl 5-gallon water bags. We would fill them from a slowly dripping faucet in the morning and hang them in the sun all day. When we returned late at night, the water and electricity were off, but we were assured of a marvelous shower before retiring. On a special shelf, we kept $700 of AIDS drugs donated by our hospital back home, to use as prophylaxis if we were cut or stabbed with a needle during surgery. This reminded us that we were playing for keeps: thankfully, no one needed the drugs. The day began with breakfast at 7 a.m., followed by chapel service at 7:30 for the hospital staff. Doctors and nurses usually presented testimony or Bible readings. The U.S. doctors sat in the back, and a member of the congregation would always come to sit behind us and translate from the native Creole into English. On the last day we were there, I mustered the courage to offer witness with translation by my friend, Dr. Jean Luis, the general surgeon. Ninety percent of the people were nominal Catholics who also practiced Voodoo; a form of African animism. Before surgery, the Catholics would offer prayers to the Christian God, and also Voodoo prayers to be certain all bases were covered. Unfortunately, the Voodoo doctors frequently were the first line of health care; patients who failed to recover from their potions and rituals were then brought to the hospital, in more serious condition. In the case of high risk pregnancy, the baby often was dead by the time a medical doctor was seen. There were many Baptist churches on the island, and Baptist missionaries ran the hospital compound. During the services we attended, I was impressed with the sincerity of the peoples' prayers and hymns and the depth of their faith. They offered thanks to God for the gifts He had bestowed upon them, meager as they were. "Amazing Grace" was easily recognized in Creole. The pastor introduced us to the congregation as the visiting American surgeons, and we received a hearty round of applause. The hospital normally had 60 beds. For two weeks before our trip, the local radio channels announced the anticipated arrival of surgeons from the U.S. Patients walked for miles to be seen; Hopital Lumiere was overflowing with dozens of patients sleeping in the halls and in the clinics. Our day ran from 8 a.m. until 5 p.m. in the operating room, a surgeon's dream. I would go for dinner at 6, and return for rounds and pre-op evaluations until 10:30 or 11 p.m. I had a group of six sixth-year medical students from Port au Prince who worked with me. They were hungry for medical education: I would teach as much as possible, especially from 10-11 p.m. One student, Rolf, spoke beautiful English and served as my translator with patients. He received one of my Leatherman Tools. The hospital had one general surgeon, two internists, a pediatrician, an obstetrician-gynecologist and several nurse anesthetists, who were excellent. They gave us unrestricted use of the four operating rooms. I had the opportunity to perform 27 urologic operations. Each day, the nurses reminded us to pray with our patients. This was not difficult, because I have been praying with my patients in Myrtle Beach for the past four years. My prayer is always very simple: "Blessed Lord, we know that you are the healer and we are the instruments of your hands. Please make the surgery go safely and smoothly for this patient. Please allow him to have a good result from what we do, and grant him the grace to accept your will. In Christ's name we pray. Amen." Surgical experiences in a Third World operating room presented unusual challenges. The temperature averaged 90 degrees. At the end of every case, we would be drenched in perspiration from the neck to the ankles. There was no reason to change scrubs, because we would be drenched again after the following case. Open windows were the only source of ventilation; the screens had holes and flies in the operating theater were common. We always irrigated well at the end of each case. The combination of patients with hearty lifestyles and few antibiotic-resistant organisms protected us from serious infections. In the States, Central Sterile Supply is always neat and well-organized; in Haiti there was chaos. Instead of instruments arranged on shelves in cabinets, there was a "central mound" two feet high and four feet wide with all of the surgical instruments. We would rummage through the inventory to find what we would need for each case. A gyn colleague, Ben Martin, had worked at Lumiere the preceding year; he donated an O'Connor-O'Sullivan retractor, which was sorely needed. By our fourth day in-country, pieces had been lost, and it was no longer functional. The hospital pharmacy was limited and disorganized; they did not have a formulary and were unsure of what medications they had available. Post-operative analgesics were almost non-existent; fortunately we brought our own supply of IV Toradol. Attempts have been made to educate the Haitians on organization and planning. Unfortunately, the culture and level of education are not conducive to outside influence, so life goes on with little change. There are so many personal stories I can relate. I was presented with a patient with kidney cancer diagnosed only by ultrasound. We performed a radical nephrectomy under the most difficult conditions. This was truly a leap in faith. There was very poor lighting in the operating room, and we had limited instruments. We fashioned a gall stone scoop to serve as a vein retractor when we had trouble identifying the renal artery. At one frustrating point in the surgery, I stepped back and prayed, "Lord, You asked me to come here to take care of your people; please guide me in this very difficult surgery." He did not let me down (I remembered the story of "Footprints" and one set of tracks in the sand). The patient did remarkably well, and I am confident he is now cured. Two women had Vesicovaginal Fistulas repaired trans-abdominally. An older man was in kidney failure with advanced prostate cancer. Most Haitians do not live long enough to develop prostate cancer. I removed his testicles and reversed his renal failure (at least temporarily). Another man had a giant hydrocele. I drained five liters of fluid from his scrotum. It is hard to imagine that he had been carrying 10 pounds of fluid between his legs for years. Benign prostatic hypertrophy was a common malady in a Third World country with few urologists. I did 14 operations on men who had been in urinary retention and wore catheters for months. These patients had very large prostate glands and usually required a TURP, a major undertaking in Haiti. Most patients were anemic and would likely require transfusion from a blood bank tainted with the threat of AIDS. Fortunately, I made use of the Indigo Laser and was able to do the surgery very safely with the newest technology. Instead of cutting away the tissue, the laser fiber was inserted into the adenoma and heat destroyed the obstructing tissue. No patients were transfused. Although the hospital staff was accustomed to postoperative hemorrhage and clot retention, they were pleasantly surprised with interstitial laser prostatectomy. The students asked if this blue box was American magic. I told them, "No, this is American Voodoo." Dr. Jean Luis was an inspiring figure. He was a tall, handsome Haitian-trained general surgeon, a compassionate physician and skilled technician who worked tirelessly for his people. In the absence of visiting specialists, he was responsible for all surgical cases that arrived at Hopital Lumiere. He was a classic general surgeon, with expertise in all surgical specialties. If he could not handle a critical case, the patient would die. When I visited, the ob-gyn surgeon was on vacation, so he was busy with Caesarian sections and vaginal deliveries. He knew details on each of the inpatients, and worked unending hours in the hospital. One morning, in chapel, we had three visiting dignitaries - ministers from surrounding provinces who came in to give sermons. I was asked to delay my surgery that morning, to attend to their urologic needs. I saw each individually in the clinic; two had come to have their Viagra prescriptions refilled. The "poster boy" of our trip was a child about 10 years old, who suffered from rickets. His femurs met the tibias at the knees at 90-degree angles. He walked with extreme difficulty on his toes. Dr. Jarrett performed rotational osteotomies on the tibia and fibula bilaterally, straightened the legs and applied external fixation, without the use of intra-operative x-ray. The boy would remain in the hospital for three months until the next orthopedic surgeon arrived, to remove the fixation and begin rehab. On a late Thursday night with my entourage, I again heard the question, "Doctor, would you see just one more patient?" They brought in a beautiful eight-month-old child with his mother. As they undressed the boy, I was the only one in the room who recognized that he suffered from the most devastating urological birth defect: exstrophy of the bladder. In this condition the bones of the pelvis fail to close and the pubic bones remain widely separated. The bladder lays open on the lower abdominal wall pouring urine. The penis and scrotum are split; epispadius leaves the urethra open on the dorsum of the penis. The testicles do not descend to the normal position. After explaining the condition to my students, I reassured Dr. Jean Luis that there was no immediate emergency. I would make sure that he would receive sophisticated surgical correction, when I returned home. I have been in contact with Dr. Charles Horton, the founder of Physicians for Peace in Norfolk, Virginia. We have now made arrangements for a department chairman of urology, who has an upcoming trip scheduled for Haiti, to perform the major reconstructive surgery in-country. On Saturday morning at 5 a.m., the four of us left for the trip home. I told Dr. Jean Luis earlier that I had expected to work very hard; I left totally drained. But what a marvelous feeling of satisfaction and inner peace. We performed 52 operations; we succeeded in clearing the hospital of all of the surgical patients who required our attention. Miraculously, no patients died, in spite of very serious diseases; we experienced no sepsis, no transfusions, no infections. I cannot recall a single complication. But then, why should I be surprised? We did the work that He called us to do. "Blessed Lord, we know that you are the healer and we are the instrument of your hands..." We returned home with many new friends and many treasured memories. I will never forget the kiss I received from the woman with urinary incontinence, or the smile on the boy with the bow legs now straight. I developed immense respect for those who devoted their entire lives to helping these less-fortunate. The Haitian people proved to be a humble but proud people, who endured the degradation of poverty and illness with grace and acceptance. Many have asked if I plan to return to Haiti. On the flight home, at a quiet time, this thought came to mind. If I am given the opportunity, as my own death is imminent, to think back on perhaps five of the most meaningful times in my life, they would be my marriage to MaryEllen, the birth of my daughter, Erin, my graduation from medical school and surgical training, and my trip to Haiti. I have no choice but to return again and again. Not because I have so much to offer, but because this opportunity has given so very much to me. I was able to see the Lord through the faces of my Haitian patients. I was given the opportunity to operate on so many desperately poor, suffering people. Remember, He told us, "As long as you do it for one of these, the least of your brethren, you do it for Me" The call to care for patients in Haiti and the Third World in general, will never be fully satisfied. All specialties are in demand. If one responds to this gentle call, the following organizations may be helpful: World Medical Mission 828-262-1980 United Methodist Volunteers In Mission sejumvim.compuserve.com Mercy Ships mercyships.org International Volunteers in Urology ivumed.org Physicians for Peace physiciansforpeace.org AmeriCares 203-966-5195 International Medical Corps 310-826-7800 Northwest Medical Teams 503-624-1000 Catholic Medical Association cathmed@cathmed.com You can reach William R. Greene, M.D., FACS at GUDOC96@HOTMAIL.COM, or by snail mail at 823 82 Pkwy. Myrtle Beach, S.C. 29572; 843 449 1010 ext. 239.
|
||