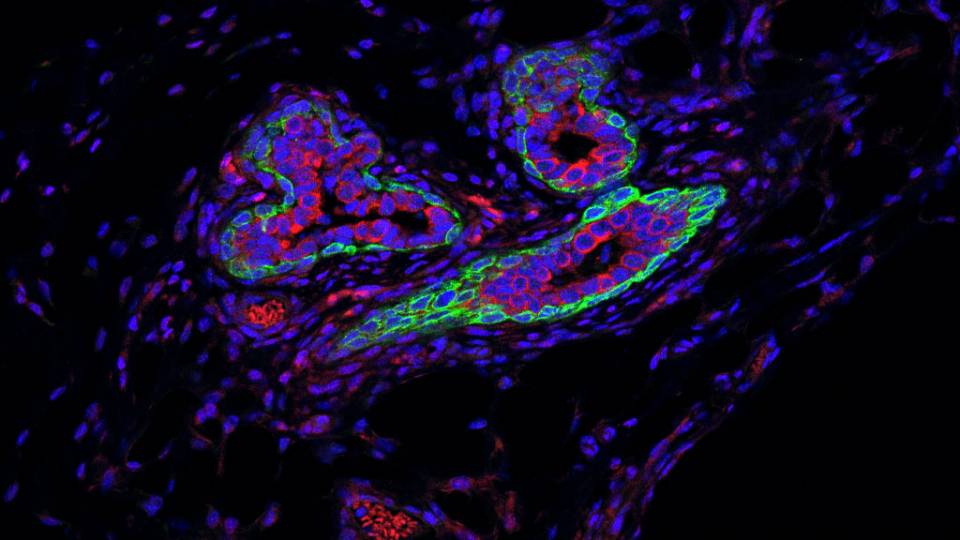
In mice and in human tissue, a new compound discovered by Yibin Kang, seen here in his lab in 2017, disables a key gene that’s implicated in breast, prostate, liver, lung, colon and other cancers.
Imagine you could cure cancer by targeting one tiny gene. Imagine that same gene occurred in every major cancer, including breast, prostate, lung, liver and colon. Imagine that the gene is not essential for healthy activity, so you could attack it with few or no negative side effects.
Cancer biologist Yibin Kang has spent more than 15 years investigating a little-known but deadly gene called MTDH, or metadherin, which enables cancer in two important ways — and which he can now disable, in mice and in human tissue, with a targeted experimental treatment that will be ready for human trials in a few years. His work appears in two papers in today's issue of Nature Cancer.
“You can’t find a drug target better than this: MTDH is important for most major human cancers, not important for normal cells, and it can be eliminated with no obvious side effects,” said Kang, Princeton’s Warner-Lambert/Parke-Davis Professor of Molecular Biology and one of the principal investigators of the Princeton Branch of the Ludwig Institute for Cancer Research.
“In the two papers we are publishing back-to-back today, we identify a compound, show it is effective against cancer, and show that it is very, very effective when combined with chemotherapy and immunotherapy,” said Kang. “Even though metastatic cancers are scary, by figuring out how they work — figuring out their dependency on certain key pathways like MTDH — we can attack them and make them susceptible to treatment.”
For years, Kang has focused on metastasis — the term for cancer’s ability to spread from one place to another in the body — because he knows that metastasis makes cancer deadly. While 99% of breast cancer patients survive five years after diagnosis, only 29% do if the cancer has metastasized, according to current numbers from the National Cancer Institute.

Minhong Shen
“Metastatic breast cancer causes more than 40,000 deaths every year in the U.S., and the patients do not respond well to standard treatments, such as chemotherapies, targeted therapies and immunotherapies,” said Minhong Shen, an associate research scholar in Kang’s lab and the first author on both papers. “Our work identified a series of chemical compounds that could significantly enhance the chemotherapy and immunotherapy response rates in metastatic breast cancer mouse models. These compounds have great therapeutic potential.”
“Yibin Kang and his team found a key to unlock a possible solution to the challenge of cancer metastasis, the primary cause of death due to cancer,” said Chi Van Dang, the scientific director of Ludwig Institute for Cancer Research. “His team was also able to devise a small, drug-like molecule to neutralize this deadly property of cancer. Though this was achieved in preclinical studies, I personally hope that their strategy will one day alter the lives of cancer patients.”
Kang holds the same hope. “While a lot of women diagnosed with early-stage breast cancer will be essentially cured with surgery and treatment, for some, maybe five, 10, 15, 20 years later, they’ll have a recurrence, often as metastatic relapse,” Kang said. “It’s a time bomb. And for scientists, it’s a puzzle. Why do you have two patients who present with the same early-stage cancer but whose outcomes are very different?”
'We kept looking until we found the key'
In 2004, the same year that Kang came to Princeton, MTDH was first identified as a gene involved in metastatic mouse breast tumors. The gene received little attention until Kang’s blockbuster 2009 paper, which showed that MTDH was amplified — meaning it produced MTDH proteins at abnormally high levels compared to normal cells — in 30 to 40% of tumor samples from breast cancer patients, and it drives metastasis and chemoresistance in those tumors.
That discovery drew media attention from around the world.
“There was a lot of excitement,” Kang recalled. “‘Wow, we found a metastasis gene related to poor outcomes in patients! What next? Can we target it?’ That was the big question, because at the time, nobody knew how this obscure, little-known gene worked. It had no similarity to any other known human protein. We didn’t know if it was important to normal physiology.”
His team's research continued, and their next set of breakthroughs, published in a series of papers in 2014, showed that MTDH is vital for cancer to flourish and metastasize. Mice without the gene grew normally, showing that it isn’t essential for normal life. And critically, if those mice did get breast cancer, they had significantly fewer tumors, and those tumors didn’t metastasize.
Kang’s team soon found that the same was true for prostate cancer and then lung and colorectal cancer. Other teams confirmed similar results for liver cancer and many other cancers.
“So basically, in most major human cancers, this gene is essential for cancer progression and all the terrible things associated with cancer, and yet it doesn’t seem to be important for normal development,” said Kang. “Mice can grow and breed and live normally without this gene, so we knew this would be a great drug target.”
Around the same time, the crystal structure of MTDH revealed that the protein has two finger-like projections that nestle into two pockets on the surface of another protein, SND1, “like two fingers sticking into the holes of a bowling ball,” Kang said. Their experiments showed how intimately MTDH and SND1 depend on each other.
That gave the researchers an idea for how to tackle MTDH, which they hadn’t been able to disable head-on: if they could disrupt this connection to SND1, that would neutralize MTDH’s dangerous effects. They pored through the molecules in the Small Molecule Screening Center, a library of compounds housed in Princeton’s Department of Chemistry, until they found a molecule that can fill one of the two deep pockets — those bowling-ball holes — thus preventing the proteins from interlocking.
“We knew from the crystal structure what the shape of the keyhole was, so we kept looking until we found the key,” said Kang.
Kang makes it sound simple, but finding the right compound was incredibly challenging, said Shen. “The screening took two years without any progress, until one day we saw a significant signal shift in our high-throughput screening assay platform. At that moment we knew the compound does exist, and we found it!”
More than a decade after confirming that MTDH would be a good target, they’d finally found the silver bullet.
Because while it’s important to show that mice born without MTDH are resistant to cancer, that doesn’t help patients, whose genes can’t be rewritten.
“In 2014, we showed what happens if you knock out a gene at birth,” Kang said. “This time, we show that after the tumor has already fully developed into full-blown, life-threatening cancer, we can eliminate the function of this gene. We found that whether you do it genetically or pharmacologically using our compound, you achieve the same outcome.”
Two mechanisms, no side effects
Kang and his colleagues have shown that MTDH has two primary mechanisms: it helps tumors survive stresses they commonly experience as they grow or under the treatment of chemotherapy, plus it muzzles the alarm cry coming from organs invaded by tumors.
Our immune system is designed for defense, not offense: If it doesn’t know a cell is an invader or is under attack, it can’t send help. The MTDH-SND1 duo suppresses the pathway that presents cancer cells’ danger signal to the immune surveillance system.
“Now, with this drug, we reactivate the alarm system,” Kang said. Subsequently, the drug makes tumors much more susceptible to both chemotherapy and immunotherapies. “In normal tissues, healthy cells are usually not under stress or presenting signals that can be recognized as foreign by the immune system, so this is why MTDH is not essential for normal tissues. In essence, MTDH is a quintessential ‘cancer fitness gene’ that is uniquely required by malignant cells to survive and thrive.”
He continued: “Internally, the tumor cell needs MTDH to survive, and externally, it needs it to hide from the immune system. So you have one drug that disables these two important mechanisms — survival and escape — of the cancer cell. And the most important thing is, the drug has very little toxicity. When we tested it in mice, there were no side effects at all. That’s the best of all worlds: two mechanisms attacking a tumor, very few side effects on normal tissues, and best of all, this is not for one specific kind of cancer, but for all major kinds of cancers.”
Seeding the world with cancer researchers
Kang knows that to tackle cancer in all its forms, the world needs more cancer researchers. “Another very gratifying part of my work is seeing these young researchers mature and make their own contributions,” Kang said. “I recently got an email from a fellow at Dana-Farber Cancer Institute, who said that my course was his first introduction to cancer biology 10 years ago at Princeton, and he’s now becoming a physician scientist.”
In addition to the students who enroll in his course “Molecular Basis of Cancer,” Kang trains the steady stream of undergraduates, graduate students and postdoctoral researchers who conduct research as part of his lab group.
“I’m lucky because I have some of the most brilliant students, and they usually join the lab as freshmen or early sophomores, and many of them stay,” he said. “By the time they graduate, many have become highly competent researchers and published papers. Some who start as pre-med convert from pure M.D. to M.D./Ph.D. because they enjoy the research so much.”
Kang always has several projects going on, but he’s had at least one upper-level scientist — and usually at least one undergraduate — working on MTDH since 2005.
“It’s the longest continuous evolving project in our lab,” he said. “Every single trainee I put on MTDH was the best student or postdoc in my lab at the time. The project is just that challenging.”
Kang compared the painstaking lab work to the endurance sports that he took up during the pandemic. “Research is like a marathon: it can be boring and lonely, and you don’t have cheerleaders, except during races,” he said. Kang completed a half Ironman in August and competed in Ironman Arizona last week.
“Students with the determination to stick to a project like this tend to be the best students,” he said. “They also get the best training from working with the toughest project. It pays off; almost every single graduate student or postdoc who worked on this project has now become a faculty member, leading their own research team.”
He pointed to Shen, who made a “heroic” contribution to both papers, Kang said.
“Minhong came to my lab in 2012 as a visiting graduate student from China. He was supposed to come for a half year, but he was so good that I asked him to stay another half year, and then I invited him back to be a postdoc. And he flourished. Born in a rural village in China, he is now going to the Karmanos Cancer Institute in Detroit, to be a principal investigator and professor. He started from a humble position — a visiting student — and ended up doing the most important work in the lab.”
Kang also came from rural China, from a coastal fishing village. “It took me a long journey to come to Princeton,” he said. “I’ve found that immigrant scientists are willing to take risks, to venture out of their comfort zone.”
That willingness has been key to his research journey, he said. “A lot of projects we take on are exciting but risky, and not following any beaten path. In Princeton, we have the flexibility of coming up with the most creative idea and then just going for it.”
Kang is at once a pure scientist, pursuing knowledge for love of it, and an applied scientist looking to solve a very real problem. That makes finding a treatment for MTDH satisfying on multiple levels, he said. “This gene is singularly important for all kinds of different cancers, and by mutating one single amino acid, we eliminate its tumor-promoting function. Nothing is purer than that. This work is both biochemistry and genetics in their most beautiful form.”
Kang and his team are working to optimize the compound to achieve higher affinity and a lower effective drug dose. “I hope we’ll be ready for clinical trials in human patients in two to three years,” he said. “In terms of the biology, I think we are only starting to scratch the surface. I foresee another decade of discovery work, so, the saga continues.”
Current and former Princeton co-authors on the new papers include: Xin Lu, Ph.D. 2010, now an assistant professor at the University of Notre Dame; Michelle Rowicki ’20, now a researcher at Novartis; Liling Wan, Ph.D. 2014, now an assistant professor at the University of Pennsylvania; Nicole Wang ’17, now an M.D./Ph.D. student at Baylor College of Medicine; senior research specialist Xiang Hang; Hahn Kim, the director of the Small Molecule Screening Center; Minhong Shen, starting as an assistant professor at Wayne State University/Karmanos Cancer Institute on Dec. 1; former postdoctoral researcher Heath Smith, now a senior scientist at AbbVie; postdoctoral research associate Yong Tang; staff scientist and lab manager Yong Wei; and former technician Min Yuan.
“Small-molecule inhibitors that disrupt the MTDH–SND1 complex suppress breast cancer progression and metastasis,” by Minhong Shen, Yong Wei, Hahn Kim, Liling Wan, Yi-Zhou Jiang, Xiang Hang, Michael Raba, Stacy Remiszewski, Michelle Rowicki, Cheng-Guo Wu, Songyang Wu, Lanjing Zhang, Xin Lu, Min Yuan, Heath A. Smith, Aiping Zheng, Joseph Bertino, John F. Jin, Yongna Xing, Zhi-Ming Shao and Yibin Kang (DOI: 10.1038/s43018-021-00279-5) and “Pharmacological disruption of the MTDH–SND1 complex enhances tumor antigen presentation and synergizes with anti-PD-1 therapy in metastatic breast cancer,” by Minhong Shen, Heath A. Smith, Yong Wei, Yi-Zhou Jiang, Sheng Zhao, Nicole Wang, Michelle Rowicki, Yong Tang, Xiang Hang, Songyang Wu, Liling Wan, Zhi-Ming Shao and Yibin Kang (DOI: 10.1038/s43018-021-00280-y), both appear in the Nov. 29 issue of Nature Cancer. The research was supported by the Brewster Foundation, Ludwig Cancer Research, the Breast Cancer Research Foundation, the National Institutes of Health (R01CA134519), Department of Defense Breast Cancer Research Program (BC151403), the American Cancer Society, Susan G. Komen (PDF17332118) and the New Jersey Commission on Cancer Research (DFHS15PPCO21). This research was also supported by the Preclinical Imaging and Flow Cytometry Shared Resources of the Rutgers Cancer Institute of New Jersey (P30CA072720).